Trauma-Induced Facial Paralysis
Our face is one of the most important areas where we both express our emotions and communicate with our environment in a healthy way. However, damage to the facial nerve as a result of sudden traumas can lead to serious problems such as inability to mimic, speech disorders and even social isolation. In the medical literature, this condition is defined as facial paralysis due to trauma. If you want to have detailed information about this condition, you can take a look at our content. We wish you all good reading and healthy days.
Anatomy and Tasks of the Facial Nerve
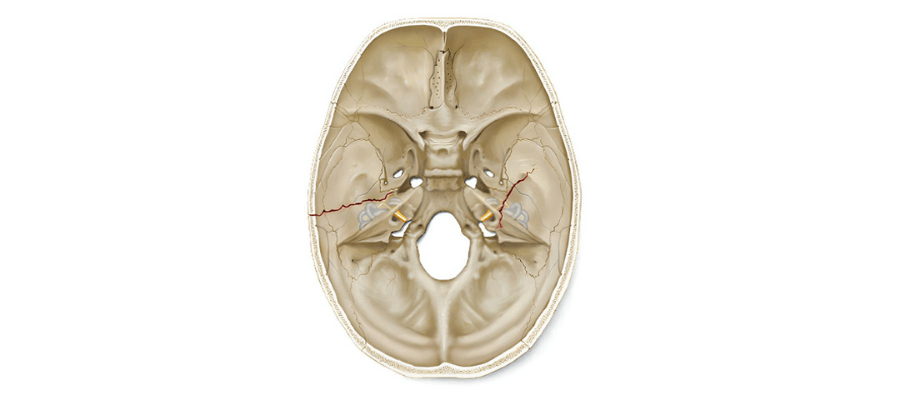
The facial nerve (Nervus facialis - 7th cranial nerve) is a mixed nerve containing both motor and sensory fibers and its main function is to provide movement of the facial muscles. In this context, it leaves the brain stem, the pons, passes between the structures of the inner ear and then travels from the skull base to the facial area to reach the facial muscles. During this progression, it is highly susceptible to trauma as it passes through several sensitive points (e.g. Fallopian canal). Therefore, through its motor fibers, mimic muscles such as the muscles of the forehead, around the eyes, mouth and lips are activated. This makes facial expressions such as smiling, raising eyebrows and blinking possible. In addition, thanks to its parasympathetic fibers, it stimulates the tear and salivary glands and transmits the sense of taste from the front 2/3 of the tongue. Accordingly, damage to the facial nerve can lead not only to impaired facial movements but also to loss of taste, dry eyes and asymmetrical facial appearance.
What is Traumatic Facial Paralysis?
Traumatic facial paralysis is a condition characterized by sudden weakness or immobility of the facial muscles that occurs when the facial nerve (nervus facialis) is damaged as a result of a physical impact or injury. This condition is usually seen as a result of traffic accidents, falls from height, sports injuries, occupational accidents, gunshot wounds or trauma caused by cutting and sharp instruments. As a result, skull fractures can cause compression or direct damage to the narrow channels through which the nerve passes. It can also be crushed, severed or trapped between swollen tissues due to impact. Therefore, traumatic facial paralysis causes serious problems both aesthetically and functionally.
Which types of trauma can cause facial paralysis?
Facial paralysis can develop due to different types of trauma, and these traumas are usually associated with damage to the areas where the facial nerve passes. One of the most common sources of trauma in this context is skull fractures and temporal bone fractures. Such fractures can cause pressure on the narrow bone canals through which the nerve passes, or direct damage to the nerve, leading to a sudden and severe onset of paralysis.
On the other hand, blunt head traumas are caused by traffic accidents, falls from a height or blows received during sports. For this reason, serious edema and contusions occur after blunt head trauma, causing pressure on the anatomical structures through which the facial nerve passes and causing paralysis.
Finally, penetrating traumas caused by objects such as glass, knives or pieces of metal penetrating directly into the face or around the ear cause a direct cut to the nerve, resulting in sudden complete paralysis. After this type of paralysis, the possibility of spontaneous recovery is very low, as the integrity of the nerve is compromised. Therefore, in facial paralysis due to penetrating trauma, the nerve may need to be surgically repaired or reconstructed using alternative treatment methods such as cross facial nerve graft.
Causes of Facial Paralysis Due to Trauma
There are certain causes of facial paralysis due to trauma. These causes usually develop due to physical damage to the areas where the facial nerve passes. In this context, the causes of facial paralysis due to trauma are as follows;
- Skull Fractures
Skull fractures are one of the most serious causes of facial paralysis due to trauma. Especially temporal bone fractures can cause nerve injury by creating pressure in the narrow bone canals through which the facial nerve passes. In this case, there may be pressure, edema or direct cutting on the nerve. In addition, since the temporal bone passes very close to the facial nerve, such fractures can cause rapid development of facial paralysis, leading to permanent damage to the nerve and the risk of complete paralysis. Therefore, early intervention is essential.
- Blunt Head Trauma
Blunt head trauma is another important cause of facial paralysis. This can occur in cases such as traffic accidents, falls from a height, sports accidents or blows to the head, causing hard blows to the head. Such traumas can also trigger intracranial edema and bleeding. Therefore, since blunt trauma usually causes temporary or permanent loss of function of the nerve rather than nerve rupture, treatment to reduce edema should be done before paralysis develops.
- Penetrating and Cutting Injuries
Another cause of facial paralysis is penetrating and sharp instrument injuries, which occur when objects such as glass, knives, metal pieces enter the facial area. This can lead to paralysis as it directly damages the facial nerves. For this reason, in case of piercing and cutting injuries, the area should be intervened quickly with nerve repair or graft procedure and the treatment process should be facilitated by reducing the risk of infection.
- Surgical Complications
Trauma-induced facial paralysis can occur as a result of accidental damage to the facial nerve during some surgical interventions. Damage to the facial nerve can occur especially during procedures performed on the head and neck region such as ear surgeries, jaw surgeries and salivary gland surgeries that are not performed with the correct methods. However, this condition generally does not occur during the surgical intervention, but in the days following the surgical intervention.
- Direct Facial Trauma
Direct facial trauma can be caused by blows to the facial area, especially the cheekbone, jaw or nose. Such traumas often cause indirect damage to the facial nerve. In such cases, surgical intervention is absolutely necessary to reduce the pressure and edema on the nerve. Thus, by restoring the function of the nerve, the risk of permanent facial paralysis can be minimized.
- Animal Bites
Animal bites, one of the most common causes today, can cause facial paralysis, especially when they hit facial nerves. At this point, deep wounds may occur and cause the risk of infection. There may also be damage or rupture of nerve tissue after the bite. Therefore, the functions of the facial muscles can be fully restored by early intervention.
- Firearm Injuries
Finally, gunshot wounds can also cause facial paralysis. Because the penetration of objects such as bullet cores or shrapnel into the facial area can cause major destruction in the area where the nerve is located. Therefore, in such cases, the wound area should be cleaned as quickly as possible and antibiotic treatment should be started quickly. In this way, the patient is protected from infectious complications and the treatment process proceeds in a healthier way.
How Does Trauma Damage the Facial Nerve?
Trauma can severely damage the facial nerve through different mechanisms and the severity of this damage varies according to the type and location of the trauma. However, the most common of these is mechanical compression. This mechanical compression occurs when edema, hematoma or bone fractures, which usually occur after head trauma, press on the narrow bone canals through which the nerve passes. In this situation, nerve conduction weakens, nerve nutrition deteriorates and degenerative processes begin over time and facial paralysis occurs.
On the other hand, a direct nerve cut, which is seen in penetrating or cutting injuries, causes the integrity of the facial nerve to be disrupted, i.e. complete rupture. This type of damage is especially common when sharp and piercing objects such as knives, glass, metal pieces or bullets directly hit the anatomical areas through which the nerve passes and completely stops the signal transmission to the facial muscles, causing sudden, complete facial paralysis.
Finally, crush or stretch-type injuries occur mostly in blunt trauma, when the nerve is squeezed between bone structures or subjected to a sudden strain. In addition, post-traumatic ischemia (impaired blood flow) can prevent the nerve from being nourished, leading to loss of function at the cellular level. As a result of such damage, nerve conduction is impaired, the necessary signals cannot be transmitted to the muscles and symptoms of paralysis of the facial muscles appear.
Symptoms of Facial Paralysis Due to Trauma
In cases of facial paralysis due to trauma, certain symptoms may occur. Since these symptoms vary completely from person to person, they may not be seen in the same severity or in the same combination in every patient. In this context, the symptoms of facial paralysis due to trauma are as follows;
- Sudden muscle weakness or immobility on one side of the face
- Inability to close the eyelid or a feeling of dryness in the eye
- Sagging of the corner of the mouth and consequent difficulty in eating or drinking
- Facial asymmetry
- Immobility of the forehead muscles
- Sudden pain in the ear or around the face
- Noticeable decrease in taste sensation
- Sensory hypersensitivity
- Tearing or dry eye conditions
- Paralysis that develops immediately after trauma or within hours
Diagnostic Methods for Facial Paralysis Due to Trauma
Early diagnosis is very important in cases of paralysis due to trauma. Because early diagnosis and intervention preserves the healing potential of the nerve and can prevent permanent damage. At this point, the diagnostic methods for facial paralysis due to trauma are as follows;
- Physical Examination and Neurologic Evaluation: First, the mobility of the patient's facial muscles is monitored and functions such as blinking, forehead wrinkling and lip movement are analyzed. In this way, it is understood whether the patient is paralyzed in the first place.
- Evaluation of Trauma History and Visual Findings: Afterwards, the type of trauma experienced by the patient (head trauma, cutting-piercing injury, animal bite, etc.) and the changes in the face after the event are examined in detail and the findings of the trauma are noted.
- CT (Computed Tomography) Scan: After preliminary evaluations, a computed tomography scan is performed to analyze the condition of the skull bones and temporal bone structures. Thus, skull fractures, inner ear structures and changes in the nerve canals are detected.
- MRI (Magnetic Resonance Imaging): Once the condition of the bone structures has been determined, a Magnetic Resonance Imaging (MRI) system is used to examine the damage rates in the tissues. Thus, edema, rupture, inflammation or tumor-like formations in the nerve are detected immediately.
- Electrophysiological Tests (EMG, ENOG):After the necessary examinations, the electrical conduction capacity of the facial nerve is evaluated. Thus, the degree of nerve damage and the potential for recovery can be easily determined.
- Yüz Siniri Fonksiyon Skalaları (House-Brackmann vb.):Finally, after the investigations and examinations, the severity of facial paralysis is classified. The house-brackman scale can be used to do this. This greatly facilitates clinical follow-up throughout the treatment process.
Treatment Methods for Facial Paralysis Due to Trauma
Many treatment methods are used in connection with trauma. These treatment methods may vary depending on the degree of damage to the facial nerve, the type of trauma, the age and general health of the patient. For this reason, while conservative treatments, i.e. medication, corticosteroid use, antiviral drugs and physical therapy are at the forefront in mild cases of paralysis, surgical interventions should be applied in cases where the nerve is completely cut and there are serious structural disorders. At this point, surgical procedures such as nerve repair with microsurgery, nerve grafting, free muscle transfer and facial suspension surgeries can be performed. However, these treatment methods should be determined with a multidisciplinary approach, in cooperation with neurology, plastic surgery and physical therapy specialists. Otherwise, the desired results may not be achieved. Therefore, you can visit our facial paralysis treatment options page for more detailed information.
What is the Main Difference Between Early (first 6 months) and Late (after 18 months) Treatment in Traumatic Facial Paralysis?
|
Status |
Early Treatment (First 6 Months) |
Late Treatment (After 18 Months) |
|
Nerve Condition |
The nerve may be alive. Therefore, function may return. |
The nerve is usually degenerated. |
|
Muscle Condition |
Muscles are functional, atrophy has not yet started. |
Muscles develop atrophy and fibrosis |
|
Treatment Objective |
Ensuring nerve recovery and functional return |
Restoring facial symmetry and aesthetics |
|
Applied Methods |
Steroid therapy, antiviral drugs, nerve repair, nerve decompression |
Free muscle transfer, facial sling surgery, plastic surgery |
|
Physical Therapy Effect |
Highly effective, supports muscle function |
Limited, muscle function may be lost |
|
Botulinum Toxin Usage |
Usually not required |
Frequently used, it is preferred to reduce asymmetry. |
|
Surgical Difficulty Level |
Less invasive interventions may be sufficient |
More complex and multi-stage surgeries may be required |
|
Chance of Success |
High; complete or near complete functional recovery can be seen |
Partial success; aesthetic and functional correction is targeted |
Following facial paralysis caused by trauma, not only physical but also psychological and social effects may occur. These effects can significantly impact an individual's self-perception, social relationships, and quality of life. Especially the loss of facial expressions can result in an inability to express emotions, which may lead to misunderstandings or social exclusion. Over time, this situation can cause the individual to withdraw, avoid social environments, and experience intense feelings of shame, paving the way for loss of self-confidence, severe anxiety disorders, and even clinical depression.
In addition to all these, some patients may also experience difficulties in their professional lives. For example, individuals working in communication-focused professions may feel inadequate due to the lack of facial expressions. Therefore, to reduce the long-term effects of such psychosocial issues, individuals should have access not only to surgical and medical treatments but also to psychological counseling and support groups. In this way, with patience and professional support, the individual's quality of life can be rebuilt.
If you would like to learn more about trauma-related facial palsy, feel free to contact Doctor Be and his team today.













